Aesthetic rehabilitation through crown lengthening laser surgery and zirconium CAD/CAM veneers: a multidisciplinary case report
Introduction
Nowadays aesthetics is paramount in all dental procedures and aesthetic rehabilitation in frontal area should be prosecuted whenever possible. Until recently it was accepted that the morphology, shape, size, proportions, colour and texture of anterior teeth is what makes the smile aesthetic. It is more appropriate to perceive teeth and gingival tissues as two parts of one and the same aesthetic complex. A combined approach including periodontal plastic surgery and prosthetic rehabilitation of aesthetically compromised teeth can help in some clinical cases to achieve harmonious smile (1).
Excessive gingival exposure or the so called “gingival smile” might be consequence from skeletal deformities, vertical excess of upper jaw, short upper lip, insufficient clinical crown length, altered passive eruption or a combination of any of the aforementioned factors (2,3). In order to determine the type of surgery to be performed, Coslet et al. classify altered passive eruption as a function of the relationship established among gums, anatomical crown, cement-enamel junction (CEJ) and alveolar crest (AC) (2). Following these parameters, they established the following types and subgroups: Type 1—there is excessive amount of gingiva; Type 2—there is normal amount of gingiva; subgroup a—the AC is normal to the CEJ; subgroup b—the AC is at the CEJ. Treatment plan is determined according to clinical type.
Important step in the treatment planning of gummy smile is also establishment of the so called supracrestal tissue attachment. It represents the distance between the bottom of the periodontal sulcus and the AC and should be 2 mm (4). Having in mind also the depth of the sulcus the clinician has to create minimum 3 mm distance from the AC to the future CEJ at the end of the surgery and respect it when considering the treatment procedure—only gingivectomy or combination of gingivectomy and osseous surgery.
Recent years different types of lasers are introduced to dentistry and applied in various procedures. Among them only the Er:YAG laser is capable of ablating not only soft but also hard tissues like enamel, dentin and bone. Thus, this is the only one laser until now that can be used in surgical crown lengthening procedure with osseous removal (5).
Bearing in mind that the main goal of every rehabilitation should be not the aesthetics only but to preserve as much as possible hard dental tissues and periodontal health, veneers are the most biological approach towards aesthetic problems. The use of 0.3–0.5 mm thick veneers preserve 95–100% of the enamel volume after the preparation, without exposing the dentin (6). Porcelain laminate veneer fabricated with conventional techniques requires an impression of the prepared teeth, an impression of the opposing arch, preparation of casts, and extensive laboratory time (7). During the prosecution of all these steps a lot of mistakes may be accumulated. Contemporary CAD/CAM systems provide complete digital workflow, high accurateness of the restorations, satisfactory aesthetic result and materials with excellent physical and mechanical properties.
The manuscript presents a case report managed by multidisciplinary treatment approach consisting of laser assisted crown lengthening procedure with osteotomy and CAD/CAM conservative zirconium veneers for the optimal correction of smile aesthetics.
Case presentation
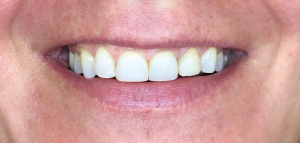
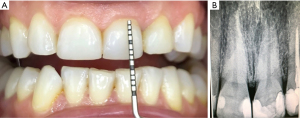
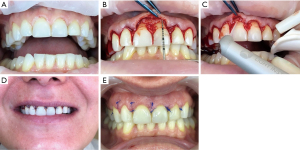
A 40-year-old female patient is referred with a chief complaint of gummy-smile and lack of aesthetics in frontal area due to multiple old composite obturations. Her dynamic smiling uncovers about 2–3 mm of gingival tissue. The gingival contour of central incisors is lower than the lateral incisors so frontal teeth appear asymmetrical. The clinical crown of central incisors is as high as wide and is not following Lombardi’s 1,618 “golden mean” ratio (8). However, the patient exhibited a slight asymmetry of the gingival margins on the upper right and left first canines and premolars, with overall gingival display (Figure 1).
The intraoral examination shows abraded cusps of both maxillary canines and tooth #13 is longer than tooth #23. The composite veneer on tooth #22 has unaesthetic appearance. The incisal edge of tooth #11 is longer and going slightly in distal direction which makes the right central incisor’s crown look bigger and buccally positioned. This may be a collateral damage of the multiple old composite fillings on both central incisors (Figure 1).
Presurgical protocol includes periodontal and radiographic examination (Figure 2). Probing pocket depth reveal 1 mm, the length of the clinical crown of central incisors—8 mm and the length of the anatomical crown of same teeth established on X-ray—11 mm. A goal of 3 mm supracrestal tooth exposure apical to the planned restoration margin is determined.
All procedures performed in the study are in accordance with the ethical standards of the institutional and/or national research committee and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient.
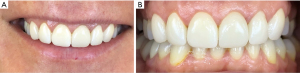
Surgical technique—gingivectomy is performed with Er:YAG laser (Lite Touch, Light Instruments, Yokneam Illit, Israel) in soft tissue mode with tip 0.6 mm and energy settings—150 mJ/15 Hz, after measuring the desired tooth length and placing bleeding points. Intrasulcular incision is performed with scalpel 15C blade and full thickness buccal flap is elevated. Bone remodeling and smoothening are done using Er:YAG laser in hard tissue mode with tip 1.3 mm and parameters of the energy—150 mJ/20 Hz (Figure 3). The flap is sutured with internal mattress and single interrupted sutures (6-0 polypropylene) and the sutures are removed 14 days after. No complications during the surgery or the healing period are registered.
After a month for recovery of the gingival tissues the prosthetic work is proceeded. The preparation design chosen for this clinical case is gingival chamfer and incisal reduction. A 2.5× magnification (Rose Microsolution, USA) is used in order to acquire better visibility and precision in this technically sensitive process (9). The buccal cut performed is in three planes (cervical, middle and incisal plane) and the depth of penetration is 0.4 mm as a minimum thickness for the zirconium material used (UTML KATANA Zirconium Disk, A1, Kurraray Noritake, Japan).
An optical impression (digital scan) of prepared teeth and the antagonists, is taken with the digital camera of Trios 3 (Trios 3Shape Inc., Denmark) with an accuracy of 4.5±0.9 µm (10). The bite registration in static and dynamic occlusion is also recorded with buccal scanning technique.
Computer-aided design of the future veneers is preformed via Trios 3Shape design software (Figure 4).
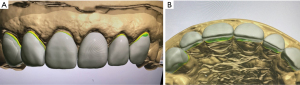
Material of choice is 19 mm height ultra-translucent multi-layered yttria-stabilized KATANA zirconia (Kuraray Noritake Dental Inc., Japan). Computer-aided manufacturing machine 5-S2 (VHF Camfacture AG) cut the restoration from zirconium disk. Veneers are glazed and sandblasted with 50 μm Al2O3 particles, 2 Bar (0.2 MPa).
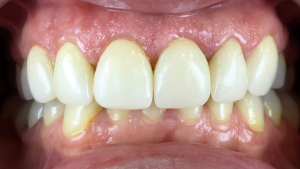
Veneers are cemented with rubber dam isolation via Panavia V5 dual—polymerisation cement (Kurraray Noritake Dental Inc., Japan) according to the manufacturer instructions and case was followed-up for 1 year (Figures 5,6).
Discussion
The expectation of an aesthetically harmonious smile increases the level of difficulty when treating patients. Laminate veneers stand out as a treatment option for cosmetic rehabilitation in clinical practice, as they are a more conservative procedure and mimic dental structures (11). Very often aesthetically harmonious smile requires surgical interventions like crown lengthening procedures with or without osseous resection to reduce the amount of the exposed gingiva and to increase the clinical crowns. When taking the decision for such procedure the clinician must follow biological principles and strict treatment plan (12). When the desired CEJ is too close to the bone crest there is not enough space for the supracrestal tissue attachment and there is risk for failure for the future restorations. In such cases after gingivectomy osseous surgery is required to establish the necessary width of 3 mm from the margin of the future restorations to the bone crest (13).
Since the Er:YAG laser is approved from FDA for bone surgery in 2004 it is used in various osseous procedures including crown lengthening (14). There are reports from the literature demonstrating lots of benefits of the laser like bactericidal effectiveness, less discomfort and vibrations to the patient, no tissue damage and healing complications, effectiveness in bone surgery (15,16). In the present study is noticed that the Er:YAG laser is effective not only in removing soft (excessive gingiva) and hard (bone) tissues, but it can be safe during the surgery without causing more bleeding or other side effects. Moreover, no complications after the surgery are observed and the results are stable during the follow-up examination (up to 1 year) (Figure 6).
Ultra-translucent multi-layered yttria-stabilized KATANA zirconia is new generation of highly aesthetic and translucent material for anterior restorations especially. It combines high profile of mechanical properties with superior optical properties (17). Clinicians all over the world are struggling to find a biomaterial to implement hardness and fracture-resistance, high aesthetics, stability of the properties, sufficient bond with hard dental tissues and if possible, to be machinable. The choice of zirconium as a biomaterial for the CAD/CAM production of veneers aimed to study if all of this requirement can be fulfilled in one single material and be applied in highly aesthetic zone as anterior region for veneers. According to the manufacturer, the presented ultra-translucent multilayered zirconia ceramic has comparable translucency to e.max Press LT (Ivoclar Vivadent, USA)—43% for KATANA versus 44% for e.max and is 30–75% stronger to e.max in a three-point bending test. One controversial point is the bonding of zirconium ceramics to hard dental tissues without retention form. The applied double-polymerizing cement ensures not only adhesive micromechanical bond but a chemical also. The MPD monomers used in the ceramic primer ensures durable bond to hydroxyapatite and zirconia, which is the greatest benefit. Further study on application of zirconia ceramics for aesthetic purposes is need in order to enlarge the variety of materials of choice for every clinician, implementing the high-technology dental milling systems. One of the crucial steps when using zirconium material is the functionalizing process or surface roughening process to increase the shear bond strength between the inner surface of the restoration and the tooth structure. Sandblasting with 50 μm Al2O3 particles is proven as one of the most successful methods of roughening the surface (18).
Cementing of anterior zirconium veneers is a crucial step in the whole technological process and it is essential to be with a material without having a tertiary amine in its composition as most of the light- curing cements. On the other side when working with zirconium there is a better bond strength when the fixating agent is dual-polymerised, but a one which is amine-reduced, amine-free and lacking benzoyl peroxide in order to achieve better colour stability (19).
A precise diagnosis and a comprehensive treatment plan that considers facial and dentogingival individual aspects should be mandatory to predict the result of an oral treatment, especially when aesthetics is involved (20).
The combination of aesthetic plastic periodontology and use of CAD/CAM technology is efficient, predictable and highly precise multidisciplinary approach towards disharmonious smile.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at https://dx.doi.org/10.21037/ht-21-4). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in the study are in accordance with the ethical standards of the institutional and/or national research committee and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Studer S, Zellweger U, Schärer P. The aesthetic guidelines of the mucogingival complex for fixed prosthodontics. Pract Periodontics Aesthet Dent 1996;8:333-41; quiz 342. [PubMed]
- Levine RA, McWire M. The diagnosis and treatment of the gummy smile. Compendium 1997;18:757-62. [PubMed]
- Konikoff BM, Jhonson DC, Schenkein HA. Clinical crown length of the maxillary ante-rior teeth preorthodontics and postorthodontics. J Periodontol 2007;78:645-53. [Crossref] [PubMed]
- Lee EA. Esthetic crown lengthening: contemporary guidelines for achieving ideal gin-gival architecture and stability. Curr Oral Health Rep 2017;4:105-11. [Crossref]
- Ishikawa I, Aoki A, Takasaki AA, et al. Application of lasers in periodontics: true innovation or myth?. Periodontol 2000 2009;50:90-126. [Crossref] [PubMed]
- LeSage B. Establishing a classification system and criteria for veneer preparations. Compend Contin Educ Dent 2013;34:104-12. [PubMed]
- Garber D. Porcelain laminate veneers: ten years later—part I: tooth preparation. J Esthet Dent 1993;5:56-62. [Crossref] [PubMed]
- Lombardi RE. The principles of visual perception and their clinical application to den-ture aesthetics. J Prosthet Dent 1973;29:358-82. [Crossref] [PubMed]
- Pecheva A, Vangelov L, Tzanova S, et al. Evaluation of the impact of optical magnifica-tion on the precision of tooth preparation for laminate veneers. IOSR-JDMS 2019;18:88-92.
- TRIOS® #1 in ADA study for trueness and precision in intraoral scanners. Accessed 20. 02. 2020. Available online: https://www.3shape.com/en/news/2015/trios-n1-in-ada-study-for-trueness-and-precision-in-intraoral-scanners
- Passos L, Soares FP, Gallo M. Esthetic Rehabilitation through Crown Lengthening Surgery and Conservative CAD/CAM Veneers: A Multidisciplinary Case Report. Case Rep Dent 2016;2016:5720851 [Crossref] [PubMed]
- Lee EA. Aesthetic crown lengthening: classification, biologic rationale, and treatment planning considerations. Pract Proced Aesthet Dent 2004;16:769-78. [PubMed]
- Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol 1961;32:261-7. [Crossref]
- Aoki A, Sasaki KM, Watanabe H, et al. Lasers in nonsurgical periodontal therapy. Periodontol 2000 2004;36:59-97. [Crossref] [PubMed]
- Yaneva B, Firkova E, Karaslavova E. Early clinical effectiveness of Er: Yag laser in as-sociation with the red complex of bacteria in the initial treatment of moderate chronic periodontitis. Acta Med Bulg 2014;41:37-44. [Crossref]
- Stübinger S. Advances in bone surgery: the Er: YAG laser in oral surgery and implant dentistry. Clin Cosmet Investig Dent. 2010;2:47-62. [Crossref] [PubMed]
- Anusavice K J. Criteria for selection of restorative materials: properties versus technique sensitivity. Quality evaluation of dental restorations: criteria for placement and replacement, 1989:15-59.
- Saleh NE, Guven MC, Yildirim G. Effect of different surface treatments and ceramic primers on shear bond strength of self-adhesive resin cement to zirconia ceramic. Niger J Clin Pract 2019;22:335-41. [PubMed]
- Alkurt M, Duymus ZY. Comparison to Color Stability Between Amine with Benzoyl Peroxide Includes Resin Cement and Amine-reduced, Amine-free, Lacking of Benzoyl Peroxide Resin Cements After Thermocycle cements. J Adv Oral Res 2018;9:24-30. [Crossref]
- Lin WS, Zandinejad A, Metz MJ, et al. Predictable Restorative Work Flow for Comput-er-Aided Design/Computer-Aided Manufacture-Fabricated Ceramic Veneers Utilizing a Virtual Smile Design Principle. Oper Dent 2015;40:357-63. [Crossref] [PubMed]
Cite this article as: Pecheva A, Yaneva B. Aesthetic rehabilitation through crown lengthening laser surgery and zirconium CAD/CAM veneers: a multidisciplinary case report. Health Technol 2021;5:15.